Your Genes and Viral Infections
Do genetic variations impact how we respond to viruses? How do individual genetics impact the severity of infection from COVID19?
Human DNA and viruses have been coevolving since millions of years. Virus-human interactions are thought to have driven as much as 30% of the human genome evolution since diverging from chimpanzees. Approximately 8% of the human DNA is from viruses - it is now integrated into our cells.
One of the earliest cases where the genetic impact was put to test was in poliovirus infections in twins. One of them was diagnosed with the paralytic form of the disease signalling a genetic influence.
Since then research has uncovered various genes playing a contributing role in the severity of a viral infection. For example, immunity related genes like HLA and their variants play a prominent role in defending against viruses. These individual genetic variants may help explain why some people infected with viruses like dengue, HIV or hepatitis B experience severe complications or progression than others who can clear the infection rather quickly and recover fast.
Can genetics explain why COVID-19 is making few people very sick while others have mild symptoms or haven’t gotten sick at all?
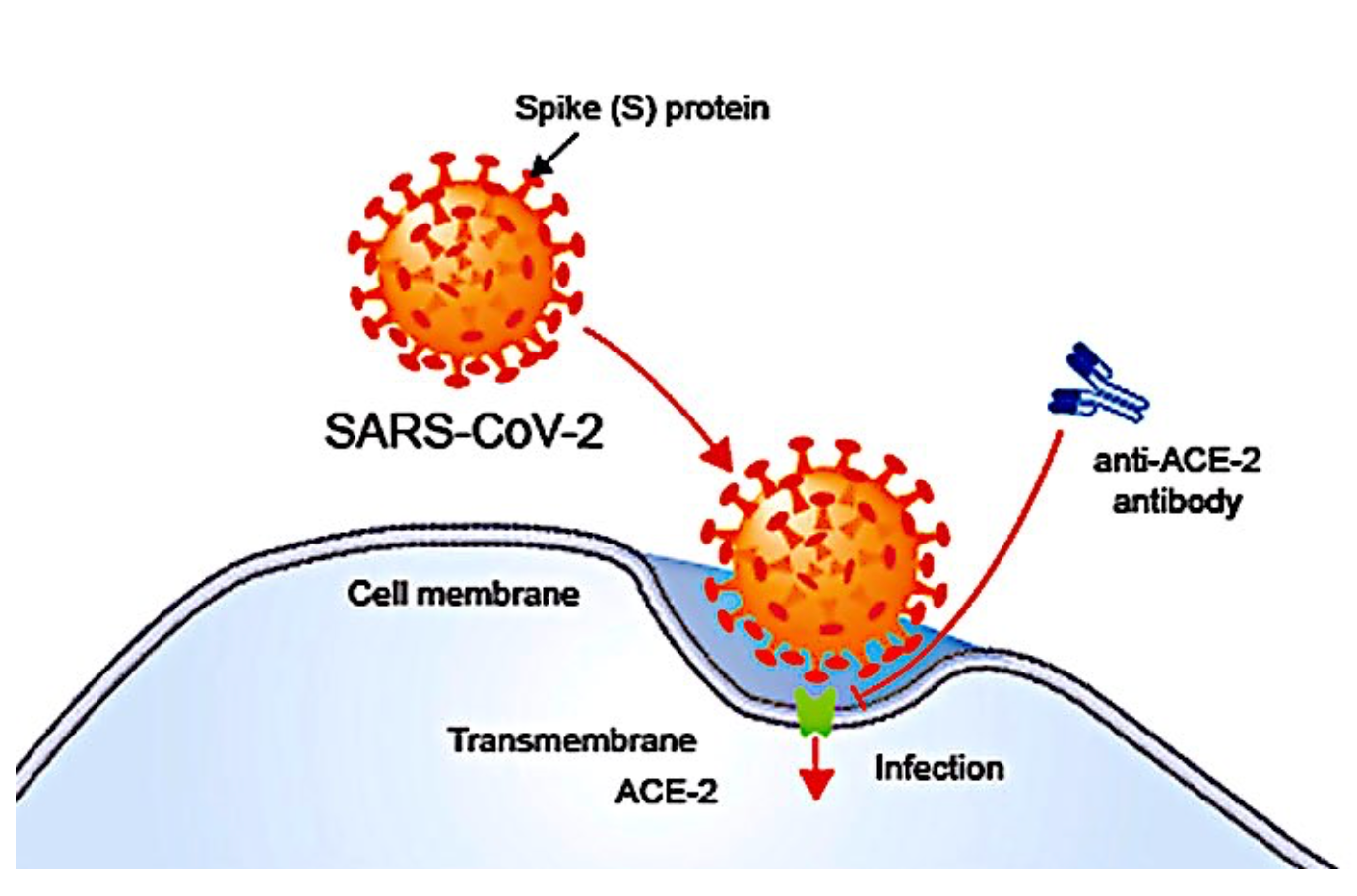
How the SARS-CoV-2 virus works
ACE2 is the entry point for this virus.
Recent research is showing that the COVID-19 virus binds to the human ACE2 receptors with high affinity. It’s gain of function enables it to get into human cells in under 30 seconds and it’s very similar to the HIV virus in that respect. Unlike the HIV virus which can only survive outside the body for 30 minutes, Sars-Cov 2 can survive on metal, glass and plastic for as long as nine days.
The spike S protein on the coronavirus acts as the key to the lock provided by the ACE2 receptor.
Once both the proteins interlock, the cell opens the door of its cell membrane and allows access to the virus.From here the virus enters the cell and fuses with its membrane. Once it’s inside the cells, the virus releases its genetic material into the cell’s nucleus, which enables it to replicate and release new virions from the cell’s surface which infect neighbouring cells.
What’s ACE2’s role in our body?
ACE2 is a receptor protein on the surface of various human cells.
ACE2 plays an important role in regulating the body’s blood pressure and fluid balance. This enzyme is found in our lungs, respiratory tract, liver, kidneys, brain and other organs.
Latest research shows that COVID19 may attack the brain too in certain cases.
Genes coding for ACE2 receptors
The ACE2 gene encodes for the ACE2 enzyme. From what we know from research so far, the ACE2 gene expression directly influences the formation of epithelial cells. These cells are the barrier between the inside and outside of the body and often the first place that a virus attacks. The variants associated with greater expression of ACE2 may provide more entry points for the virus.
The adult bronchial tree in our lungs is covered in a continuous layer of epithelial cells. They are central to the defenses of the lung against viruses and environmental contaminants.
This may be surprisingly why the respiratory tract is a major site of SARS-coronavirus (CoV) infection and disease morbidity.
While the genetic basis of ACE2 expression and function and how it varies by different populations is largely unknown, research shows the number of ACE2 variants are significantly more common in east asian populations (95% of people have it) compared to other groups. Some of these SNPs include rs4646127, rs2158082, rs5936011, rs6629110, rs4830983, and rs5936029. In contrast, less than 65% of European populations carry this major allele.
Interventions and nutrients to target
Now that we’re aware of the role of ACE2 as the primary protein through which COVID19 gains access to cells, potential drug interventions may target these proteins. Interventions being considered seeks to inhibit the virus’ ability to replicate and block it from binding to ACE2 receptors.
There are still no answers yet but we will know more as more data gets available.
Our immune system makeup is a function of our environment, stress, diet, genetics and other factors. In old age the antibodies per milliliter of our blood goes down due to lower NK cells (natural killer cells) and the immune system is not well regulated. When the COVID-19 virus infects an older person, their bodies are subjected to cytokine storms and their immune system doesn’t know when to break instead of accelerate. This is the reason why older individuals and immunocompromised people are at high risk.
These are the nutrients that helps regulate our immune function:
Vitamins
Vitamins A, C, D and E are known to support immune system health. Vitamin C is far more than just a “vitamin” - it is a foundational molecule that protects and regulates every cell, and one of the most effective antiviral agents known. While there is no evidence that it can help prevent COVID-19, it can potentially help make the illness shorter and milder.
Vitamin A could potentially be a supportive nutrient to protect barrier function, But animal studies suggest that the ACE2 receptor may be upregulated by all-trans retinoic acid, a vitamin A derivative. So you should be careful while consuming it when infected by COVID-19.
Other nutrients and bioactive compounds that can help
Selenium: A potent antioxidant and a cofactor of glutathione peroxidase, an important antioxidant enzyme. A deficiency of selenium can alter the immune response and increase the pathogenicity of a virus.
Potassium: Not likely to be a preventive strategy. May be especially beneficial in severe cases when the patient becomes hypokalemic due to excessive potassium loss.
Zinc: May improve the chance of avoiding respiratory tract infections in the elderly and those who are zinc deficient.
Melatonin: Melatonin and its metabolites have been shown to have immunomodulatory and antioxidant properties by scavenging free radicals and by upregulating antioxidant pathways.
The best approach is to know your individual deficiency risks and nutrient targets and get the best combination through food and multivitamin supplements to ensure you are providing the right environment to your cells.
You can use Gini’s health tracker to figure out if you're meeting your daily gene adjusted macro and micronutrient needs to support your immune system.
The future
The ongoing research on the genetics of infectious diseases and the rapid growth of the people who are DNA tested will shed more light on the virus - human gene interactions. This can be used to identify people who are extremely susceptible to the virus and may experience severe symptoms ahead of time. It can also be beneficial in crafting more personalized strategies for vaccinations, dietary interventions and treatments.
You can help us in collecting more data about COVID , genetics and lifestyle by linking your data to Gini Health and answering these questions.